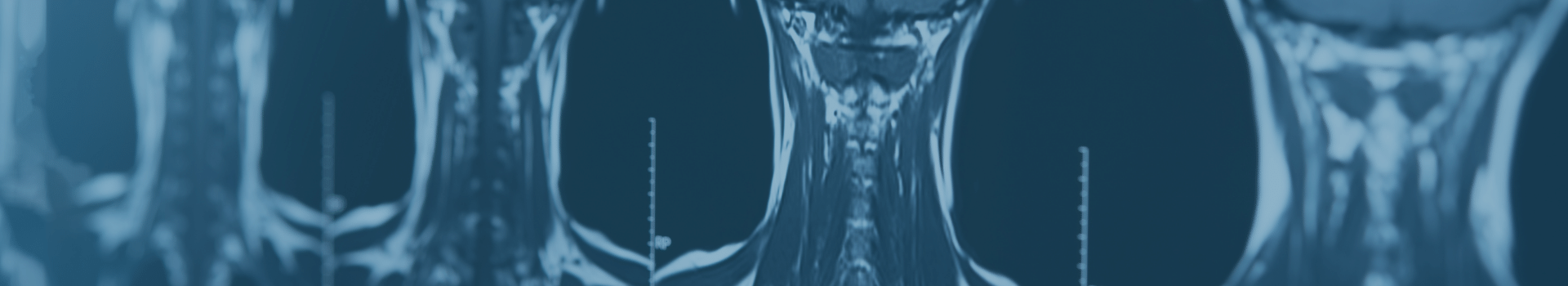
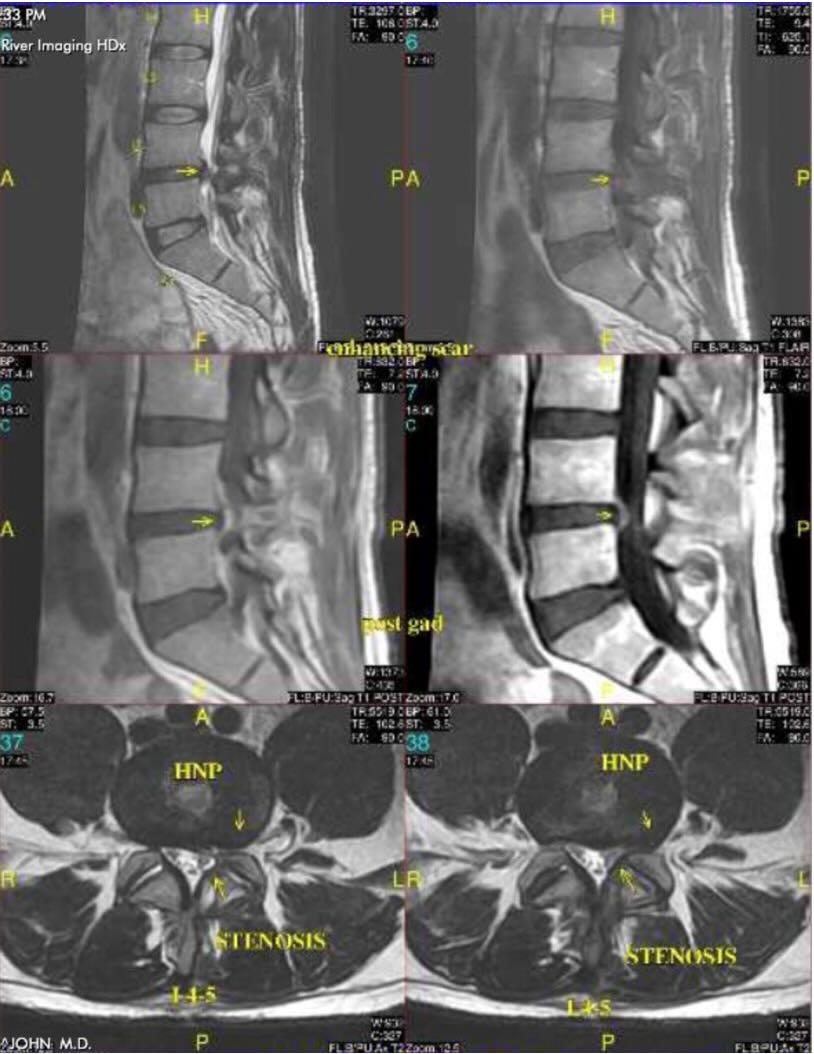
Lumbar Radiculopathy is usually due to a lumbar disc herniation or foraminal stenosis. A lumbar disc herniation is when a small piece of lumbar disc material herniates from its normal location and compresses the nerve or the thecal sac. The most common areas for disc herniation are the lower two disc spaces, L4-5, and L5-S1. L4 is the superior bone and L5 is the inferior bone, with the disc denoted as the space in between or the L4-5 disc; the same notation for L5-S1 and any other disc. If the disc herniates laterally, it will compress a nerve, usually causing unilateral leg pain; if the disc herniates centrally, it usually causes back and sometimes bilateral leg pain. When there is a disc herniation at L4-5 to one side or the other, a patient can develop a foot drop from compression of the L5 nerve. A foot drop occurs when you lose the ability to lift your foot up while taking a step, and the foot then drags as you walk. An L4-5 disc herniation can cause severe leg pain starting in the buttocks radiating to the top of the foot with or without a foot drop. An L5-S1 herniation can cause severe leg pain starting in the buttocks radiating to the bottom of the foot with or without weakness when stepping down. A herniated disc at L3-4 will cause thigh pain and at L2-3 will cause groin pain. Most symptomatic disc herniation resolves on their own over time, and it is predicted that only 10 – 15% of patients actually will need surgery.
Foraminal stenosis causes similar symptoms as a disc herniation, but the cause is much different. In foraminal stenosis, there is facet joint degeneration, causing compression around the nerve as it exits from the spinal canal. There can be a contributing disc herniation in addition to foraminal stenosis, making the symptoms worse. The diagnosis is made using an MRI to determine if there is disc, arthritis, or both causing the symptoms.
Treatment
Non-operative. The initial course of treatment after the diagnosis has been made is oral steroids, rest, and non-steroidal anti-inflammatory agents. Once the pain has lessened, you may be referred for a course of Physical Therapy. Other options include an epidural injection to help with the pain.
Surgery. Patients are referred to a surgeon if there is a persistent weakness that does not improve after 8 –12 weeks or the pain is intolerable. Surgery includes a Micro-Foraminotomy where the arthritis is removed through a small incision (1.5 inches), takes approximately 45 minutes, and patients go home the same day.